Prisma Health shares how omicron sets new precedent for employers
Molly Hulsey //January 24, 2022//
 Thousands of South Carolina businesses readied themselves for the Occupational Safety and Health Administration’s large employer testing and vaccine mandate before the U.S. Supreme Court shut it down Jan. 13.
Thousands of South Carolina businesses readied themselves for the Occupational Safety and Health Administration’s large employer testing and vaccine mandate before the U.S. Supreme Court shut it down Jan. 13.
However, the omicron variant, which made up close to 70% of all Upstate cases the week of Jan. 10, renders testing and vaccination less of a guarantee that employees aren’t harboring the virus.
“The positivity rate in the asymptomatic community is astronomical,” Dr. Wendell James, Prisma Health-Upstate, said during a virtual meeting Jan. 13, adding that about 45% to 50% of tests from asymptomatic people are coming back positive. “That level of positivity is truly breathtaking, when you look at the potential effects that it can have on the Upstate health care system.”
That week at Prisma Health, hospitalizations jumped by 51%, representing an all-time high for COVID-19 patients.
“Over the last several days, not just across the nation, but across the state of South Carolina and in the Upstate, we have seen the numbers of these COVID patients rise at a rate that is near vertical,” said James.
A nightmare for HR
That’s not to say the COVID-19 vaccine — including the booster — isn’t doing its job, Dr. Rachel Brown, medical director of Prisma’s Business Health Solutions, told GSA Business Report.
The vaccinated are much less likely to be hospitalized during a time when 85% of hospital beds across the state are occupied, 27% filled by COVID-19 patients, according to data from the S.C. Department of Health and Environmental Control.
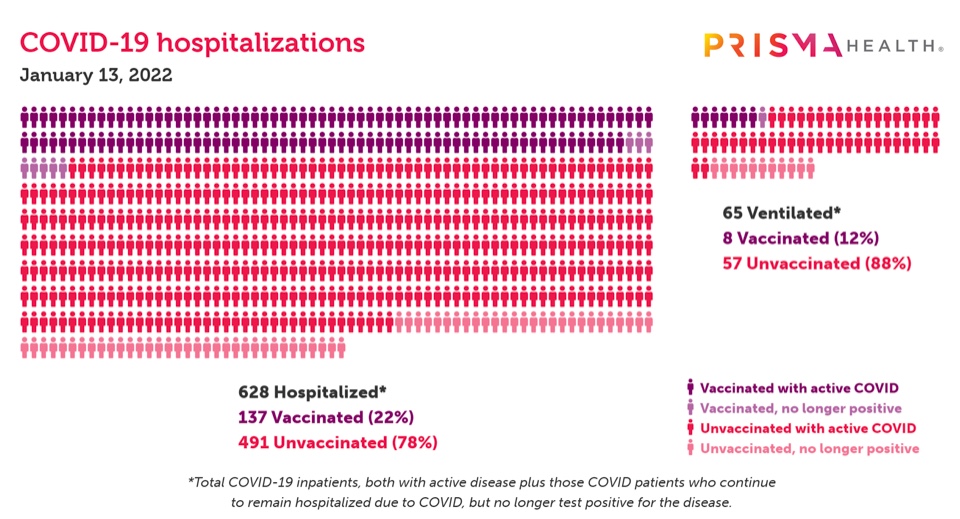
Across Prisma facilities, 78% of the 628 patients hospitalized and 88% of the 65 ventilated patients with COVID-19 were unvaccinated, according to Jan. 13 data.
But even boosted employees have a 30% chance of getting and transmitting the omicron variant, which is two to three times more infectious than the delta variant, according to Brown.
People with COVID-19 are infectious one to two days before they start showing symptoms — which may be before they test positive for the virus.
“That does not mean that three days after someone develops symptoms that they are no longer infectious,” she said.
Or that when employees receive a positive PCR test, the test is always picking up an active infection.
“Testing can be so difficult to get and resulting can take so long that often someone has passed their quarantine or isolation time by the time they get their tests,” she said, adding that some PCR tests can remain positive up to three months, even after infection has subsided.
Employers should advise their employees to return to the office or factory floor five days following the first day they stop showing symptoms and to wear a mask for another five days after returning, she said. Those who are asymptomatic but came in direct contact with a positive case should be asked to quarantine for five days following exposure and return with a negative PCR test taken on day four or afterward.
But, she warned, instituting return-to-work testing for all employees can be “a nightmare for HR,” where persistent positives prevent a workforce from returning long after recovery.
“This is so important for our supply chain and for our workforce, to get them back into the workplace as soon as they are feeling better,” Brown said. “For someone who has COVID and who is in isolation, we do not recommend a test to return to work.”
Test shortages are so severe now, she — and many of her clients — doubted that the OSHA emergency temporary standard could have even be carried out if passed.
“We are trying so hard to get organizations to understand that ordering those return-to-work tests for folks who have been out with COVID, they clog up the health care system, they use up coveted tests, and they will complicate the return-to-work picture,” she said. “So just use the clinical guidelines to bring people back to work.”
Not yet endemic
“This is a phenomenal oversimplification,” Brown said, after walking through the ways omicron is a different animal from its predecessors.
Still, Prisma’s Business Health Solutions advises businesses to make use of all the public health tools in the belt to mitigate COVID-related absences: encouraging vaccination and masking across the board during the surge. For those unable to wear masks or those operating in a workplace where feasible, social distancing can do a great deal, she said, as can proper ventilation and cleaning areas.
And events may be best put on a raincheck for the time being. Those able to work from home at Prisma Health are remote again, and even small in-person meetings have been curtailed.
“Trying to keep people separate until this surge is over is just one more important piece of the layers of risk mitigation that they can employ,” she said.
Echoing the Centers for Disease Control’s masking update on Jan. 14, Prisma Health also suggests that employers encourage the use of surgical masks, KN95, N95 or double masks where possible.
At Prisma, a spokesperson for the health care system said the company required team members in acute-care settings to wear N95 and KN95 masks when entering patient care areas and surgical masks in other areas of the hospital. At physician practices, employees must wear a well-fitting surgical, N95 or KN95 mask.
As of yet, COVID-19 is neither endemic nor a seasonal bug, but some experts believe the milder cases and the speed of infection presented by omicron may point toward that direction, especially as omicron cases begin to drop in the Northeast just weeks after it arrived on American shores.
“But this sort of ebb and flow that we’re seeing is really unique, and so it makes it difficult to predict what is next,” Brown said. “I’m not even going to try to do that.”


















